Rectal prolapse surgery is a procedure to repair rectal prolapse, which occurs when the last part of the large intestine (the rectum) stretches and protrudes from the anus. Surgery puts the rectum back in place. In this article, you will get informative knowledge about Rectal prolapse surgery by Pritish Kumar Halder.
There are a number of ways to do rectal prolapse surgery. Your surgeon will suggest the appropriate one for you based on your condition and your overall health.

Rectal prolapse surgery
Why it’s done
Rectal prolapse surgery is performed in people troubled by the pain and discomfort caused by rectal prolapse as well as the chronic symptoms that can accompany it, such as leakage of stool, inability to control bowel movements (fecal incontinence) or obstructed bowel movements. The problem is most common in older women, but it can also occur in men.
Rectal Prolapse Causes

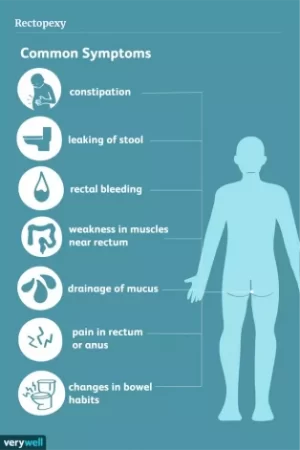
Rectal Prolapse symptoms
A variety of things can cause the condition, including:
- Long-term history of diarrhea or constipation
- Long-term history of having to strain when you poop
- Old age, which weakens muscles and ligaments in the rectal area
- Previous injury to the anal or hip area
- Nerve damage that affects your muscles’ ability to tighten and loosen, which could be caused by pregnancy, vaginal childbirth complications, anal sphincter paralysis, or injury to your spine or back
- Neurological problems, such as spinal cord disease or spinal cord transection.
Risks
Rectal prolapse surgery carries serious risks. Risks vary, depending on surgical technique. But in general, rectal prolapse surgery risks include:
- Bleeding
- Bowel obstruction
- Damage to nearby structures, such as nerves and organs
- Infection
- Fistula — an abnormal connection between two body parts, such as the rectum and vagina
- Recurrence of rectal prolapse
- Sexual dysfunction
- Development of new or worsened constipation
Rectal Prolapse Diagnosis
Your doctor can do a rectal exam. While you may hesitate to do this, your doctor may ask you to sit on a toilet and poop or at least try to go. This is helpful because it allows your doctor to see the prolapse.
You may need some other, more advanced tests to diagnose rectal prolapse, especially if you have other related conditions:
- Anal electromyography (EMG):This test checks to see if nerve damage is causing your anal sphincter problems.
- Anal manometry: A thin tube is inserted into your rectum to test muscle strength.
- Anal ultrasound: A probe inserted into your anus and rectum is used to examine muscles and tissues.
- Pudendal nerve terminal motor latency test: It checks your pudendal nerves, which you use to control bowel movements.
- Proctography:X-ray videos of your rectum during a poop show how well it holds and releases feces.
- Colonoscopy: A long tube inserted into your rectum with a tiny camera at the end can show the inside of your intestines and look for any problems that may be causing your prolapse.
- Proctosigmoidoscopy:This test also uses a long tube with a camera on the end. It’s inserted deep into your intestines to look for inflammation, scarring, or a tumor.
- MRI: Imaging scan examines all of the organs in your pelvic area.
How you prepare
To prepare for rectal prolapse surgery, your doctor may ask that you:
Clean with special soap. Before your surgery, you’ll be asked to shower using antiseptic soap to help prevent germs on your skin from causing infection after your surgery.
Stop taking certain medications. Depending on your procedure, you may be asked to stop taking certain medications.
You’ll spend one or more days in the hospital after rectal prolapse surgery. So that you’ll be as comfortable as possible during your stay, consider bringing:
- Personal care items, such as your toothbrush, hairbrush or shaving supplies
- Comfortable clothes, such as a robe and slippers
- Entertainment, such as books and games
Before the procedure
Rectal prolapse surgery can be done through the abdomen (rectopexy) or through the region around the anus (perineum).
Which approach your surgeon uses depends on a number of factors, such as the size of your prolapse, your age, other health problems, your surgeon’s experience and preferences, and equipment available. No procedure is considered the best overall. Discuss your options with your surgeon.
Rectal prolapse surgery requires anesthesia. Some options include general anesthesia, in which you’re asleep, or a spinal block, in which your lower half is numb.
During the procedure
Types of rectal prolapse surgery:
Rectal prolapse repair through the abdomen. Using an incision in the abdomen, the surgeon pulls the rectum back in place. Using sutures or a mesh sling, he or she anchors the rectum to the back wall of the pelvis (sacrum). In some cases, such as a long history of constipation, the surgeon removes a portion of the colon.

Rectal prolapse repair through the abdomen
Laparoscopic rectal prolapse surgery. Also done through the abdomen, this procedure uses several smaller incisions. The surgeon inserts special surgical tools and a tiny camera through the abdominal incisions to repair the rectal prolapse.

Laparoscopic rectal prolapse surgery
Robotic surgery. This type of surgery is similar to the laparoscopic approach but uses the assistance of a surgical robot.

Robotic surgery
Rectal prolapse repair through the area around the anus (perineal rectosigmoidectomy). During the more commonly performed form of this procedure (Altemeier procedure), the surgeon pulls the rectum through the anus, removes a portion of the rectum and sigmoid and attaches the remaining rectum to the large intestine (colon). This repair is typically reserved for those who are not candidates for open or laparoscopic repair.
Another method for repairing a rectal prolapse through the perineum (Delorme procedure) is more typically done for short prolapses. The lining of the rectum is removed and the muscular layer folded to shorten the rectum.
If you have rectal prolapse and certain other conditions, such as vaginal prolapse or pelvic organ prolapse, you might have both repairs done in one surgery.
After the procedure
You’ll spend a brief time in the hospital recovering and regaining your bowel function. You’ll begin by drinking clear liquids and transition to solid foods. The amount of time you spend in the hospital, possibly just overnight, will depend on which procedure you have.
Your doctor is likely to recommend drinking lots of fluids, using stool softeners, and eating a fiber-rich diet in the weeks after surgery to avoid constipation and excessive straining that can lead to recurrence of the rectal prolapse. Most people are able to return to normal activities within 4 to 6 weeks after surgery.
Results
For most people, rectal prolapse surgery relieves symptoms and improves fecal incontinence and constipation. However, in some cases, constipation can worsen or become a problem when it wasn’t one before surgery. If you have constipation before surgery, talk to your doctor about ways to relieve it.
Recurrence of rectal prolapse after surgery occurs in about 2% to 5% of people. It appears to be slightly more common in people who have the perineal procedure compared with an abdominal one.
Reference
https://www.mayoclinic.org/tests-procedures/rectal-prolapse-surgery/about/pac-20384704