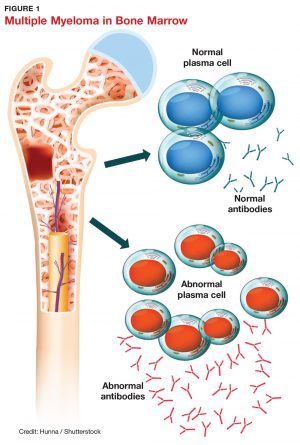
With multiple myeloma, your immune system takes a serious hit. That makes it much harder for you to fight infections. So your immune system is a focus in many treatments.

Multiple Myeloma
Harnessing the immune system to fight diseases is called immunotherapy. There are many immunotherapy drugs your doctor will consider. You’ll want to get familiar with what they do and how they work.
Immunotherapy boosts the body’s natural defenses in the fight against cancer. Some immunotherapy drugs boost the immune system to help the body fight the disease. Other suppress it to do the same thing. Still more destroy cancer cells directly or ease the side effects of other treatments.
Read the full article with PK Halder and get knowledgeable points about multiple myeloma.
Immunomodulators
These medicines recognize cancer cells. They help your immune system point out and attack those cells. The three medications below are taken as pills. Your doctor may call them immunomodulators or immune-modifying drugs.
Thalidomide (Thalomid) lowers the blood supply to cancers. It was first used to treat myeloma in the late 1990s. Before that, it was used as a sedative and nausea medication for pregnant women until it was found to cause birth defects.
Lenalidomide (Revlimid) was designed to be a stronger form of thalidomide.
Pomalidomide (Pomalyst) is the newest drug of this type approved by the FDA for multiple myeloma. It’s similar to the others above. You’re most likely to get it if you’ve received at least two prior treatments for multiple myeloma.
These drugs share a few common side effects:
- Low blood counts: These drugs can lead to conditions like:
- Anemia (a lack of red blood cells), which can leave you feeling tired and weak, among other problems
- Leukopenia, a low white blood cell count, which can make it hard to fight infections
- Neuropathy: Nerve damage can cause various things, from a pins-and-needles feeling to severe pain in your arms and legs.
- Blood clots: You’re more likely to get blood clots that can travel to your lungs from your leg.
Each drug also has more side effects that your doctor will discuss with you.

CAR T-cell Therapy
CAR T-cell Therapy
Chimeric antigen receptor (CAR) T-cell therapy involves versions of your T cells (white blood cells that fight disease) that have had their genes changed so they attach to cancer cells.
You might get idecabtagene vicleucel (Abecma), also called ide-cel, if you’ve tried at least four other types of treatment.
Interferon
This drug boosts the immune system and encourages healthy cells to move toward the cancer cells to destroy them.

Interferon system
It is injected into the skin two to three times a week. You may feel flu-like symptoms after it’s given to you.
Monoclonal Antibodies
These are human-made. They’re supposed to work on one type of target.
Daratumumab (Darzalex) attaches to multiple myeloma cells. It’ll kill them and signal your immune system to attack them. You get this treatment if other ones haven’t worked. You may have a reaction a few hours after getting the drug. This reaction may make you cough, wheeze, or have trouble breathing. You might also have a runny nose and headache. You could even get a rash. If one of these happens to you, your doctor may adjust your dose or frequency or add another medicine to lessen or stop your symptoms.

Monoclonal Antibodies
Elotuzumab (Empliciti) works in much the same way as daratumumab. It could make you cough, wheeze, or have trouble breathing. You might also have a runny nose and headache and fever or get a respiratory tract infection. You could even get a rash. You might feel super tired or have weakness or numbness in your hands and feet. And you might have diarrhea.
Isatuximab (Sarclisa) also binds to myeloma cells and kills them. This is for people who have tried at least two different treatments before this one. You could have a reaction after this drug, as well. You could have trouble breathing, a cough, chills, or nausea. Other common side effects include diarrhea, pneumonia, anemia (low red blood cell count), upper respiratory infection, and thrombocytopenia (low blood platelet count).
Clinical Trials
There are some types of immunotherapy in development. You may want to ask your doctor about joining a clinical trial so that you can try them. These include:
Adoptive T-cell transfer: This process uses your body’s T cells to destroy the cancer.
Checkpoint inhibitors: Drugs that reverse the checks and balances function in your immune system. They can turn on functions that are shut off (like stopping cancer cell growth) and turn off others (like the ones that help cancer cells grow.
Cytokines: These messenger molecules control immune system growth and activity.
Monoclonal antibodies: These human-made molecules target antigens, or substances that make your immune system react, on tumors.
Oncolytic virus therapies: These treatments use a modified virus to kill cancer cells and boost your immune response against the cancer.
Vaccines: They work like more-common vaccines to jump-start the immune system to attack cancer cells.
Reference
https://www.webmd.com/cancer/multiple-myeloma/multiple-myeloma-immunity-drugs#1