Seizures are changes in the brain’s electrical activity. These changes can cause dramatic, noticeable symptoms or no symptoms at all.
Read the full article with Pritish Kumar Halder and explore the symptoms of a severe seizure which include violent shaking and a loss of control. Because some seizures can lead to injury or be a sign of an underlying medical condition, it’s important to seek treatment if you experience them.
What are the types of seizures?
The three major types are focal onset seizures, generalized onset seizures, and unknown onset seizures.
Focal onset seizures

Focal onset seizures
Focal onset seizures occur in only one area of the brain. People may also refer to these as partial seizures.
Focal onset seizures can start in small areas of the brain, such as a single lobe, but can affect large areas.
Medical professionals typically split focal onset seizures into two types: focal aware seizures and focal awareness-impaired seizures.
Focal aware seizure
During a focal aware seizure, you’ll remain fully conscious and be aware that something is happening, even if you do not recognize it as a seizure.

Focal aware seizure and Focal impaired-awareness seizure
The symptoms of a focal aware seizure will depend on which part of the brain the seizure starts.
Focal aware seizures may be singular events but can also develop into other types of seizures. For this reason, people often refer to them as warnings or auras.
Focal impaired-awareness seizure
This type of seizure affects your consciousness. During a focal impaired-awareness seizure, you may not be able to move, talk, or hear as you did before. You may also not be able to remember the event.
Focal impaired-awareness seizures can last for up to 2 minutes. This type of seizure typically affects a larger portion of the brain than focal aware seizures.
Generalized onset seizures
These seizures start in both sides of the brain simultaneously. Among the more common types of generalized onset seizures are:
- Tonic seizures will result in your muscles stiffening up.

Generalized onset seizures
- The convulsions in clonic seizures may cause abnormal, jerky movements of your limbs. You will likely lose consciousness during these seizures that can last for a few minutes.
- Tonic-clonic. Tonic-clonic seizures include a combination of both tonic and clonic symptoms.
- During a myoclonic seizure you may experience sudden muscle spasms. These are typically too short lived to affect consciousness and pass quickly. Myoclonic seizures may be of generalized onset as well as focal onset.
- People may also refer to these as petit mal seizures. Absence seizures last for only a few seconds. They can cause you to blink repeatedly or stare into space. Other people may mistakenly think you’re daydreaming.
- During atonic seizures your muscles suddenly go limp. Your head may nod, or your entire body could fall to the ground. Atonic seizures are brief, lasting about 15 seconds. People may refer to these seizures as drop attacks.

Unknown onset seizures
Unknown onset seizures
Sometimes no one witnesses the beginning of a seizure.
For example, someone may wake up in the middle of the night and observe their partner having a seizure.
This often means there’s insufficient evidence for medical professionals to diagnose the root cause of a seizure.
In these instances, they will define the seizure as an unknown onset
seizure.
What are the symptoms of a seizure?
You can experience both focal and generalized seizures simultaneously, or one can happen before the other. The symptoms can last anywhere from a few seconds to several minutes per episode.
Sometimes symptoms occur before the seizure takes place. These can include:

symptoms of a seizure
- a sudden feeling of fear or anxiousness
- a feeling of being sick to your stomach
- dizziness
- a change in vision
- a jerky movement of the arms and legs that may cause you to drop things
- an out-of-body sensation
- a headache
- deja vu
Signs that indicate a seizure is in progress include:
- losing consciousness, followed by confusion
- having uncontrollable muscle spasms
- drooling or frothing at the mouth
- falling
- having a strange taste in your mouth
- clenching your teeth
- biting your tongue
- having sudden, rapid eye movements
- making unusual noises, such as grunting
- losing control of bladder or bowel function
- having sudden mood changes
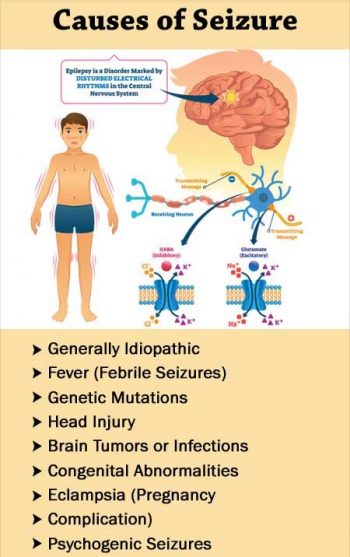
What causes seizures?
Seizures can stem from several health conditions. Anything that affects the body also may disturb the brain and lead to a seizure. Some examples include:
- alcohol withdrawal
- a brain infection, such as meningitis
- a brain injury during childbirth
- a brain defect present at birth
- choking
- substance use
- substance withdrawal
- an electrolyte imbalance
- electric shock
- epilepsy
- extremely high blood pressure
- fever
- head trauma
- kidney or liver failure
- low blood glucose levels
- a stroke
- a brain tumor
- vascular abnormality in the brain
Seizures can run in families. Tell your doctor if you or anyone in your family has a history of seizures. In some instances, especially with young children, the cause of the seizure may be unknown.
What are the effects of seizures?
Living with epilepsy and experiencing repeated seizures can have both short- and long-term effects. These can range from a drop in quality of life to increased risks of mental health conditions.
Short-term effects
Some seizures can cause you to lose total control of your body. This can lead to falls and other movements that can result in injury.
People with epilepsy typically have more physical issues, such as bruising and fractures, than people without the condition.
Being prone to seizures may also affect your quality of life. For example, you may no longer be able to drive. You may want to avoid situations where a seizure could cause serious harm, such as swimming or traveling alone.
It’s important to wear a medical identification bracelet that tells emergency responders that you have epilepsy.
Long-term effects
If you don’t get treatment for seizures, their symptoms can become worse and progressively last longer. Prolonged seizures can lead to coma or death.
While death as a direct result of seizures is rare, the risk of premature death in people with epilepsy is up to three times higher than in the general populace.
Living with epilepsy and seizures can also have an impact on your mental health. People with epilepsy have a higher rate of bipolar disorder and depression than people without the condition.
How are seizures diagnosed?
Doctors can have a difficult time diagnosing seizure types. Your doctor may recommend specific tests to accurately diagnose a seizure and help ensure that the treatments they recommend will be effective.
Your doctor will consider your complete medical history and the events leading up to the seizure. For example, migraine, headaches, sleep disorders, and extreme psychological stress can cause seizure-like symptoms.
Lab tests may help your doctor rule out other conditions that can cause seizure-like activity. The tests may include:
- blood testing to check for electrolyte imbalances
- a spinal tap to rule out infection
- a toxicology screening to test for drugs, poisons, or toxins
An electroencephalogram (EEG) can help your doctor diagnose a seizure. This test measures your brain waves. Viewing brain waves during a seizure can help your doctor diagnose the type of seizure.
Imaging scans such as a CT scan or MRI scan can also help by providing a clear picture of the brain. These scans allow your doctor to see abnormalities like blocked blood flow or a tumor.
How are seizures treated?
Treatments for seizures depend on the cause. By treating the cause of the seizures, you may be able to prevent future seizures from occurring. The treatment for seizures due to epilepsy include:

Medications
Medications
Anti-epileptic drugs are often the first treatment option for people experiencing multiple seizures. They target the signaling activities in specific brain cells and can effectively control seizures in approximately 70 percent of cases.
There are multiple types of anti-epileptic drugs. You and your doctor may have to work to find out which is the best medication for treating your condition.
Brain surgery
Doctors may recommend surgical options for treating epilepsy and seizures if medications do not work.

Brain surgery
Surgical procedures to treat epilepsy include:
- resective surgery
- multiple subpial transection
- hemispherectomy
- corpus callosotomy
Brain surgery for epilepsy can improve quality of life but does carry a risk of complications. Consult with your doctor to discuss whether surgery is the right option for you.
Nerve stimulation
In addition to brain surgery, surgeons can insert nerve stimulation devices in the body to treat epilepsy.
Vagus nerve stimulation involves placing electrodes around the vagus nerve in your neck and a generator for these electrodes in the upper chest. These devices then stimulate the nerve with electrical signals, which can help manage seizures.

nerve stimulation
Responsive neurostimulation systems also work by stimulating the brain to manage seizures. Doctors can program these devices to assess and respond to nerve activity associated with seizures, often stopping them.
These less invasive surgical options can help safely reduce seizure frequency and severity.
Doctors may also suggest deep brain stimulation therapy. This is where a surgeon places electrodes onto the thalamus.
The thalamus is a part of the brain that processes signals from almost every sensory system. It regulates consciousness, alertness, and sleep cycles.
Electrical signals from these electrodes help regulate the excitability of certain parts of the brain. This can help reduce the frequency of seizures.
Diet changes
Dietary changes may help people manage epilepsy and reduce seizure frequency long term.
If anti-epileptic drugs don’t work, following a ketogenic diet can be an alternative to surgery for some people living with epilepsy.
Multiple studies have linked the diet to positive outcomes in symptom management. However, the exact reasons why it helps people with epilepsy are not known.
However, the ketogenic diet and its variants can feel restrictive. Following the diet long term may be challenging for some.
Be sure to check in with your doctor before starting a new diet, especially as a mode of treatment.
Reference
https://www.healthline.com/health/seizures#treatment